Neuro-ophthalmology Question of the Week: Hallucinations and Illusions 1
Questions:
1. What is the difference between a hallucination and an illusion?
2. Are isolated visual hallucinations common in psychiatric disorders?
3. What is the Pulfrich effect?
4. What is the Charles Bonnet syndrome?
5. Which dementias may be associated with paranoid hallucinations and illusions?
6. What is the duration of migraine with visual aura episodes?
7. What is the duration of visual phenomenon of occipital seizures?
8. What is peduncular hallucinosis and where is its lesion?
Neuro-ophthalmology Questions of the Week: Hallucinations and Illusions 1
Neuro-ophthalmology Questions of the Week: Specific Disorders of Higher Cortical Function
Questions:
1. What is the Balint syndrome and where is its lesion?
2. What is the Gerstmann syndrome and where is its lesion?
3. What is hemineglect and where is its lesion?
4. What are the symptoms of posterior cortical atrophy and where is its lesion?
5. What are the visual symptoms of Alzheimer disease and when in the course of the disease are they likely to occur?
6. What visual symptoms may occur in Creutzfeldt–Jakob disease?
Neuro-ophthalmology Questions of the Week: Terms – Disorders of Higher Cortical Function
Questions:
1. What are the names and functions of the 2 visual higher cortical function processing streams?
2. What are the findings in a patient with alexia without agraphia?
3. Where is the lesion in alexia without agraphia?
4. What is prosopagnosia?
5. What is visual object agnosia?
6. What is optic aphasia?
7. What is topographagnosia?
8. What is akinetopsia?
9. What is simultagnosia?
10. What is ocular apraxia?
Neuro-ophthalmology Questions of the Week: Idiopathic Intracranial Hypertension (IIH)
Questions:
1. What are the symptoms of IIH?
2. What are the criteria for the diagnosis of IIH?
3. What is the ideal test when evaluating a patient with presumed papilledema?
4. A patient with papilledema has a normal brain MRI, what test should be done next?
5. What should one consider if the headaches of IIH do not improve (at least transiently) after lumbar puncture?
6. What does a normal Brain MRI in the setting of papilledema suggest?
7. What should be evaluated next in a patient with bilateral swollen discs, normal BP, normal CT with and without contrast, LP opening pressure >250mm and normal or abnormal CSF contents?
8. What should be evaluated next in a patient with bilateral swollen discs, normal BP, normal MRI with and without contrast, LP opening pressure >250mm and normal or abnormal CSF contents?
9. What are the main factors associated with IIH?
10. What condition can cerebral venous thrombosis mimic?
11. What can early recognition of cerebral venous thrombosis prevent?
12. Should papilledema from a meningeal process or cerebral venous thrombosis be classified as IIH?
13. What are the goals of the management of IIH?
14. What is basis for management of IIH?
15. What MRI findings are supportive of the diagnosis of IIH?
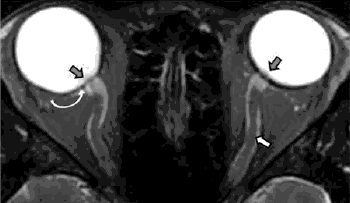
Cardinal features of superior oblique myokymia: An infrared oculography study
Recommended Reading
Question: What are the cardinal features of superior oblique myokymia?
Answer: There are 6 cardinal features of eye movement abnormality in superior oblique myokymia including:
1) involuntary intorsion and torsional oscillations;
2) episodic events lasting seconds;
3) worsening with infraduction and abduction positions that require activation of the superior oblique, and improvement with supraduction and adduction positions where the superior oblique is not activated;
4) overshooting of saccades on infraduction;
5) extorsion and diminished oscillations that were unmasked upon removal of a visual target, consistent with underlying weakness; and
6) improvement with membrane stabilizers used to treat neuropathic conditions. These features localized the lesion to the trochlear nerve, fascicle, or nucleus but not to the superior oblique muscle or neuromuscular junction.
Neuro-ophthalmology Questions of the Week: Papilledema
Questions:
1. What visual symptoms may patients with papilledema report?
2. When is central visual acuity loss experienced in papilledema, early or late?
3. What type of visual field defect is found initially with papilledema?
4. What type of visual field loss is experienced in long-standing papilledema?
5. Can visual loss from papilledema happen with any cause of papilledema?
 1
1
Neuro-ophthalmology Questions of the Week: Evaluation of Disc Edema
Questions:
1. Once optic disc edema is confirmed, what should be determined?
2. In anterior optic neuropathy with disc edema is visual acuity usually decreased?
3. In papilledema is visual acuity usually decreased?
4. In anterior optic neuropathy with disc edema is color vision usually decreased?
5. In papilledema is color vision usually decreased?
6. What are the usual characteristics of visual field defects in anterior optic neuropathy with disc edema?
7. What are the usual characteristics of visual field defects in papilledema?
8. Is anterior optic neuropathy with disc edema usually unilateral?
9. Is papilledema usually unilateral?
10. What findings are often associated with papilledema?
11. Does the absence of disc edema rule out raised intracranial pressure in a patient presenting with headache?
12. Does the absence of spontaneous retinal venous pulsations at the disc rule-out elevated intracranial pressure?
 1
1
Neuro-ophthalmology Question of the Week: Differentiating Disc Edema from Pseudoedema
Question:
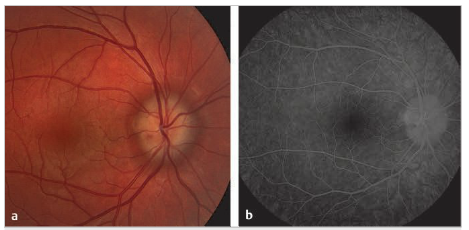
Which of the following are indicative of pseudoedema of the optic disc rather than disc edema?
1. Sharp disc margins
2. Obscured vessels
3. Venous dilation and tortuosity
4. Peripapillary hemorrhages and exudates
5. Leakage on fluorescein angiogram
6. Anomalous retinal vasculature (arterial branching)
 1
1
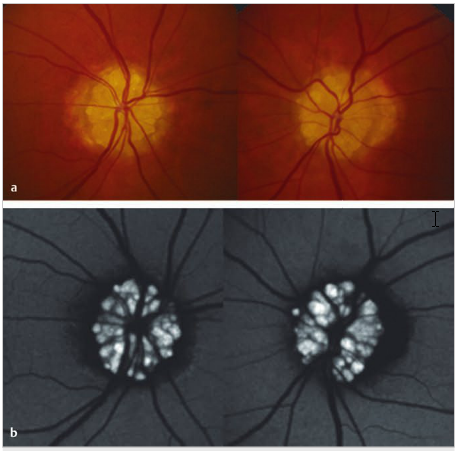
Neuro-ophthalmology Questions of the Week: Optic Nerve Anomalies
Questions:
1. How frequently are drusen present in the general population?
2. What techniques may be useful to demonstrate buried disc drusen?
3. What should be done with symptomatic patients with optic disc drusen?
4. What test should be done in all patients with optic nerve hypoplasia?
5. When is a visual field defect expected to be seen with intraocular myelination?
6. What visual field defect would be most likely with intraocular myelination?
7. What test should be done in patients with optic disc coloboma or the “morning glory” disc anomaly?
8. What visual field defect may be associated with tilted discs?
9. What findings are likely with an optic disc pit?
 1
1
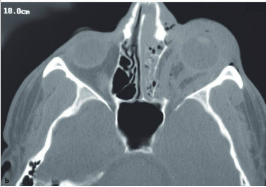
Neuro-ophthalmology Questions of the Week: Traumatic Optic Neuropathy
Questions:
1. What should be checked on all head trauma patients?
2. What are the mechanisms of traumatic optic neuropathy?
3. What imaging should be ordered when traumatic optic neuropathy is suspected?
4. What treatment is usually required for direct traumatic optic neuropathies?
5. What treatment is usually required for indirect traumatic optic neuropathies?
 1
1
